
Alert: Common Nerve Pain Medication Linked to Increased Risk of Dementia?
Alert: Common Nerve Pain Medication Linked to Increased Risk of Dementia?
In an era where neurological conditions are on the rise, a groundbreaking study has sounded the alarm on a connection between a widely prescribed medication and the risk of developing dementia. What makes this particularly concerning is that millions of people rely on this drug not just for pain, but for various "off-label" uses.
Gabapentin: From Pain Relief to Cognitive Concern
Gabapentin is an FDA-approved prescription drug primarily used to treat nerve pain and control seizures. However, because it is considered less addictive than opioids, it is frequently prescribed by doctors for conditions such as:
-
Fibromyalgia and sciatica.
-
Insomnia, anxiety, and hot flashes.
-
Chronic lower back pain.
While seen as a safer alternative for pain management, recent research published in Regional Anesthesia & Pain Medicine has shed light on the potential long-term shadows cast by this medication.
Research Findings: The Alarming Statistics
The study, led by experts at Case Western Reserve University, analyzed data from over 26,000 adults within the TriNetX health research network. Researchers tracked individuals dealing with chronic pain over a 10-year period, comparing those taking Gabapentin with a control group who were not.
The results revealed that patients who received six or more Gabapentin prescriptions faced:
-
A 29% higher risk of developing dementia.
-
An 85% higher risk of Mild Cognitive Impairment (MCI).
Perhaps most shocking was the impact on the 35–49 age group. In this demographic, the risk of dementia doubled, and the risk of MCI tripled. This is highly unusual, as neurodegenerative issues are typically expected in patients over the age of 65.
How Might Gabapentin Affect the Brain?
Nafis B. Eghrari, the lead author of the study, noted that there is still a significant gap in understanding exactly how Gabapentin influences neurodegeneration.
The drug is known to cause short-term side effects like dizziness, fatigue, and memory problems. Experts worry that long-term, high-dose usage may interfere with how brain cells communicate, potentially leading to the shrinking of specific brain areas—a hallmark of Alzheimer’s and other forms of dementia.
Differing Perspectives and Study Limitations
Despite the worrying data, other medical experts urge a cautious interpretation. Dr. Tara Spires-Jones from the University of Edinburgh pointed out that the study did not account for physical activity levels. Patients with severe chronic pain requiring heavy medication are often less active—and a sedentary lifestyle is a well-known risk factor for dementia.
Furthermore, Professor Ian Maidment from Aston University emphasized that this study shows an "association" rather than "causation." This means that while a link exists, it doesn't yet prove that the drug directly causes the brain to decline.
Practical Advice for Patients and Caregivers
While the debate continues, the study authors recommend several proactive steps:
-
Regular Cognitive Exams: Physicians prescribing Gabapentin for chronic pain should perform cognitive screenings as part of routine check-ups.
-
Monitor Mental Clarity: Patients should immediately report symptoms like sudden confusion, forgetfulness, or slowed thinking to their doctor.
-
Explore Alternatives: Do not stop taking prescribed medication abruptly. Instead, discuss non-drug pain management therapies or alternative medications with your healthcare provider.
Dementia is often an irreversible journey; therefore, prevention remains the ultimate priority. Understanding the long-term impact of the medications we put into our bodies is the first step toward lifelong brain health.
News in the same category


Experience the Gentle Wellness Benefits of Bay Leaf and Clove Tea

Foods That Support Cellular Health and Overall Well-Being in Older Adults

Doctors Reveal What Happens If You Eat Carrots Daily

Doctors Reveal That Eating Papaya Can Cause…

Doctors Reveal That Eating Cucumbers Daily Can Cause Surprising Changes in Your Body

Cloves: A Natural Ingredient That May Help Support Nail Care

Rediscover Natural Vitality at Any Age: The Surprising Pair of Coffee and Garlic

3 Vitamins That May Support Kidney Function and Help Manage Proteinuria Naturally 🌿

Banana Peel and Natural Ingredients for Wart Care: A Gentle Home Approach

To Pull or Not to Pull? The Surprising Truth About Wisdom Teeth as a "Spare Part" for Your Smile

A Spoonful of This Natural Blend May Help Support Eye Health and Reduce Eye Fatigue

Doctors Reveal That Eating Grapes May Offer Powerful Health Benefits
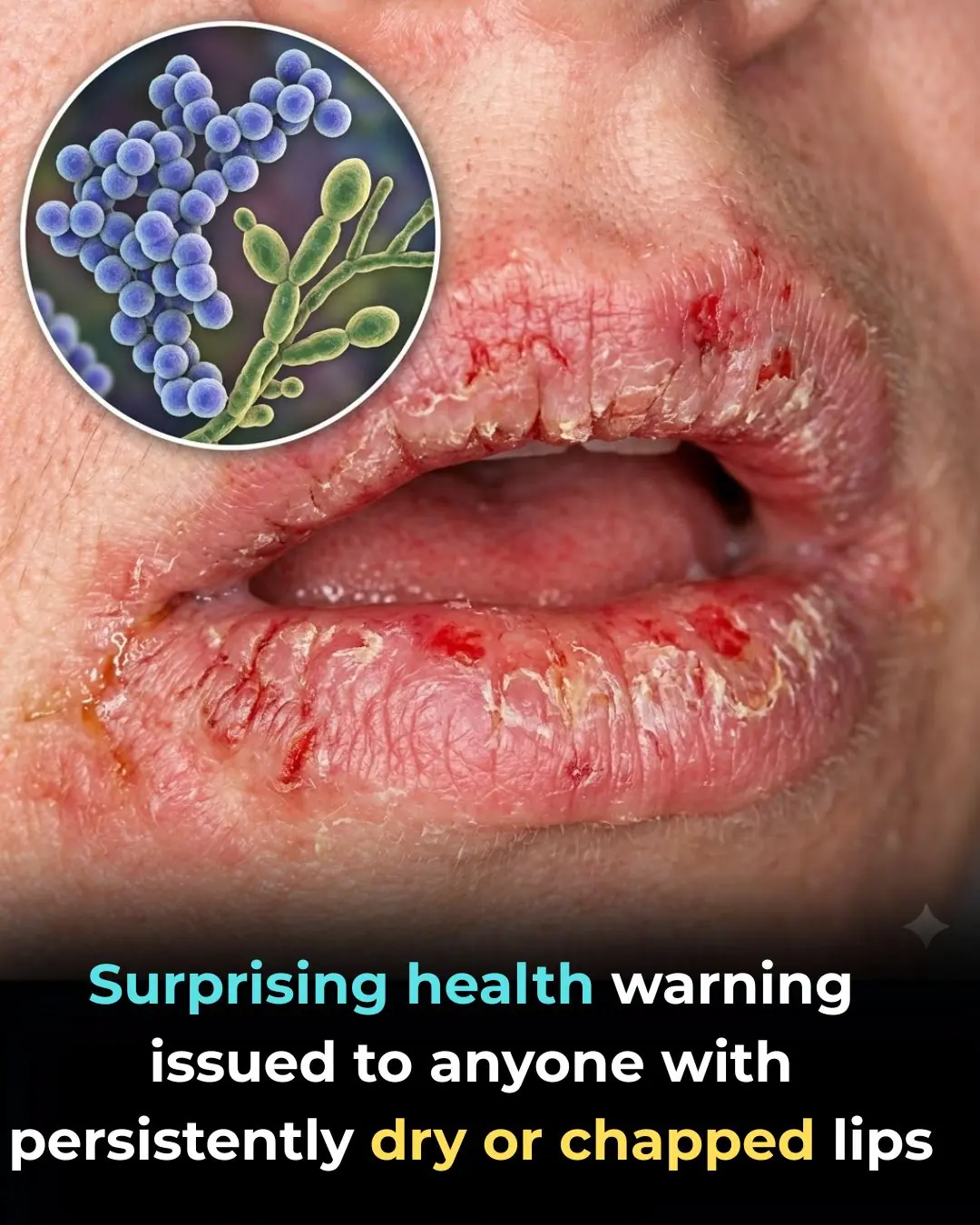
The Unexpected Health Warning You Shouldn’t Ignore If Your Lips Are Always Cracked or Dry

7 Things That Happen to Your Body When You Eat Beef Jerky Often

Eating a Clove of Garlic Every Morning: The Secret to Transforming Your Health in 6 Months

7 Things That Happen to Your Body When You Eat Beef Jerky Often

What Happens to Your Body When You Eat Watermelon?
News Post

Poor Mechanic Boy Took the Beating Meant for a Hells Angel Wife, Left For Dead, Became AFFA Same Day

Cops Beat Black Elderly Woman, Then She Makes A Phone Call to Her Son, A Delta Force

I found out my husband booked a candlelit dinner for his mistress — so I reserved the next table and brought her husband with me. He turned pale when I said, “Don’t worry, we won’t interrupt your night.”

The billionaire arrived home earlier than expected, and what he saw his housekeeper doing with his children made him cry…

YOUR 8-YEAR-OLD SAYS HER BED FEELS “TOO SMALL” EVERY MORNING… THEN YOU CHECK THE 2 A.M. SECURITY FOOTAGE AND YOUR HEART BREAKS IN SILENT TEARS

My sister gave birth, so my husband and I went to the hospital to visit her. But after seeing the baby, my husband suddenly pulled me out of the room. “Call the police right now!” I was confused and asked, “Why?”

My neighbor kept telling me she saw my daughter at home during school hours—so I pretended to leave for work and hid under her bed. What I heard next made my blood run cold.

The Best Way To Use Vaseline and Lemon on Skin for Dark Spots, Wrinkles & Glowing Skin

Pregnant Woman Was Stranded in a Snowstorm A Hells Angel Made a Call That Saved Two Lives

Experience the Gentle Wellness Benefits of Bay Leaf and Clove Tea

Foods That Support Cellular Health and Overall Well-Being in Older Adults

Doctors Reveal What Happens If You Eat Carrots Daily

Doctors Reveal That Eating Papaya Can Cause…

Doctors Reveal That Eating Cucumbers Daily Can Cause Surprising Changes in Your Body

My Uncle Raised Me After My Parents Died – Until His Death Revealed the Truth He'd Hidden for Years

“MY HUSBAND WAS CHEATING ON ME! THE HUSSY LIKED TO SWIM IN THE POOL. SO, I PUT A…”

Cloves: A Natural Ingredient That May Help Support Nail Care

Rediscover Natural Vitality at Any Age: The Surprising Pair of Coffee and Garlic

3 Vitamins That May Support Kidney Function and Help Manage Proteinuria Naturally 🌿
