
Tonsilloliths: A Comprehensive Clinical Overview of Tonsil Stones
Tonsilloliths: A Comprehensive Clinical Overview of Tonsil Stones
Tonsilloliths, commonly referred to as tonsil stones, are a frequent yet often misunderstood condition affecting the palatine tonsils. While usually benign, they can cause significant localized discomfort and social anxiety due to persistent halitosis. Understanding the pathophysiology, diagnostic nuances, and the spectrum of therapeutic interventions is essential for both patients and clinicians.
1. Anatomy and Pathophysiology: How Tonsil Stones Form
To understand tonsilloliths, one must first examine the micro-anatomy of the palatine tonsils. These lymphoid tissues are characterized by deep, convoluted invaginations known as tonsillar crypts.
The primary function of these crypts is to increase the surface area for the immune system to sample pathogens entering the oral cavity. However, this structure also creates "pockets" where organic and inorganic materials can accumulate:
-
Cellular Debris: Desquamated epithelial cells from the lining of the crypts.
-
Microbial Biofilms: A complex ecosystem of aerobic and anaerobic bacteria (such as Actinomyces and Fusobacterium).
-
Food Particles: Microscopic remnants trapped during deglutition.
-
Calcification: Over time, inorganic salts—primarily calcium phosphate and magnesium carbonate—precipitate into these organic matrices, leading to the formation of hardened "stones."
2. Clinical Manifestations and Symptoms
Small tonsilloliths are often asymptomatic and are discovered incidentally during routine dental exams or imaging. However, larger or more numerous stones can present with a variety of symptoms:
A. Halitosis (Chronic Bad Breath)
This is the most hallmark symptom. The anaerobic bacteria within the stone produce Volatile Sulfur Compounds (VSCs) like hydrogen sulfide and methyl mercaptan, which emit a distinct, pungent odor that is often resistant to standard mouthwashes.
B. Tonsillar Hypertrophy and Inflammation
The presence of a foreign body in the crypts can trigger a localized inflammatory response, leading to swelling or a sensation of fullness in the back of the throat.
C. Dysphagia and Odynophagia
Large calcifications may interfere with the normal movement of the pharyngeal muscles, making swallowing uncomfortable or painful.
D. Referred Otalgia
Because the tonsils share neural pathways (the glossopharyngeal nerve) with the ear, some patients experience "phantom" ear pain despite having no middle-ear pathology.
3. Differential Diagnosis: Distinguishing Stones from Infection
It is critical to differentiate tonsilloliths from other pharyngeal conditions to ensure appropriate treatment:
| Condition | Primary Indicators | Differentiation |
| Tonsillitis | Fever, sore throat, redness. | Usually bacterial or viral; requires antibiotics/rest. |
| Streptococcal Pharyngitis | High fever, white exudate (pus). | Exudate is liquid/creamy, unlike the solid nature of stones. |
| Tonsillar Malignancy | Asymmetrical swelling, weight loss. | Requires urgent biopsy if a lesion is fixed or ulcerated. |
4. Therapeutic Strategies: From Home Care to Surgery
Management of tonsilloliths depends on the severity of the symptoms and the frequency of recurrence.
Level 1: Conservative Home Management
For minor cases, mechanical removal and improved hygiene are often sufficient:
-
Low-Pressure Irrigation: Using a water flosser or a curved-tip syringe to gently flush the crypts.
-
Mechanical Expression: Using a cotton swab to apply gentle pressure around the crypt to dislodge the stone.
-
Saltwater Gargles: A solution of warm water and salt can help reduce inflammation and alter the pH of the oral environment to discourage bacterial growth.
Level 2: Medical Interventions
If halitosis is the primary concern, clinicians may recommend:
-
Oxygenating Mouthwashes: Products containing chlorine dioxide or zinc can neutralize VSCs.
-
Topical Antibiotics: Occasionally used to reduce the bacterial load, though not a long-term solution.
Level 3: Surgical and Advanced Procedures
When stones are chronic and severely impact quality of life, surgical intervention may be warranted:
-
Coblation Cryptolysis: This procedure uses radiofrequency energy to "smooth" the surface of the tonsil, effectively closing the deep crypts while leaving the tonsil tissue mostly intact.
-
Laser Tonsil Cryptolysis: A CO2 laser is used to vaporize the edges of the crypts, eliminating the pockets where stones form.
-
Tonsillectomy: The definitive "cure." By removing the tonsils entirely, the source of the crypts is eliminated. This is typically reserved for severe, recurrent cases due to the recovery time involved for adults.
5. Prevention and Long-Term Oral Health
Preventing the formation of tonsilloliths centers on disrupting the biofilm and keeping the crypts clear:
-
Meticulous Oral Hygiene: Brushing the tongue and the very back of the palate helps reduce the bacterial load.
-
Hydration: A dry mouth (xerostomia) allows bacteria to flourish. Consistent water intake promotes saliva production, which has natural antimicrobial properties.
-
Post-Prandial Gargling: Rinsing the mouth with water after meals can prevent food particles from settling into the tonsillar folds.
Conclusion
While tonsilloliths are rarely a medical emergency, they represent a significant nuisance for those who suffer from them. By understanding the underlying anatomy and the calcification process, patients can take proactive steps toward management. If conservative methods fail, modern medical technology offers minimally invasive options like cryptolysis to provide long-term relief without the necessity of a full tonsillectomy.
News in the same category


Waking Up Between 3 and 5 AM: What It Really Means for Your Body and Mind

Why Cottage Cheese Deserves a Spot in Your Daily Diet

Who Is Most at Risk of Night Cramps?

Are Sprouted Potatoes Safe to Eat
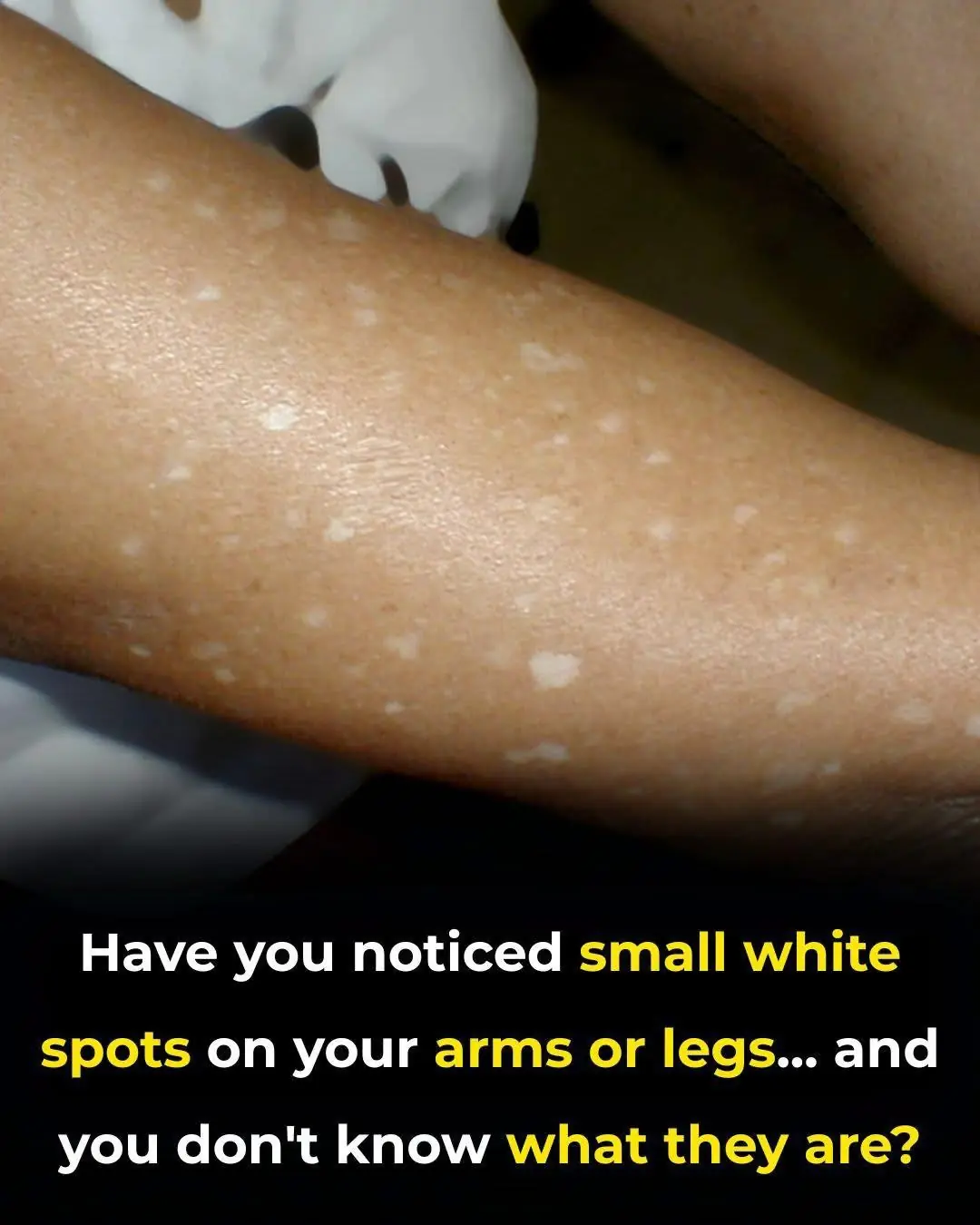
Have You Noticed Small White Spots on Your Arms or Legs? Here's What They Are

Avoid Ginger If You Have These 5 Health Problems

Why Daily Showers After 65 May Do More Harm Than Good

Health Benefits of Eating Garlic Before Bed

What Your Partner Does Every Day Could Quietly Affect Your Health

Everyone Does This Wrong: The Hidden Truth About Washing Strawberries Properly
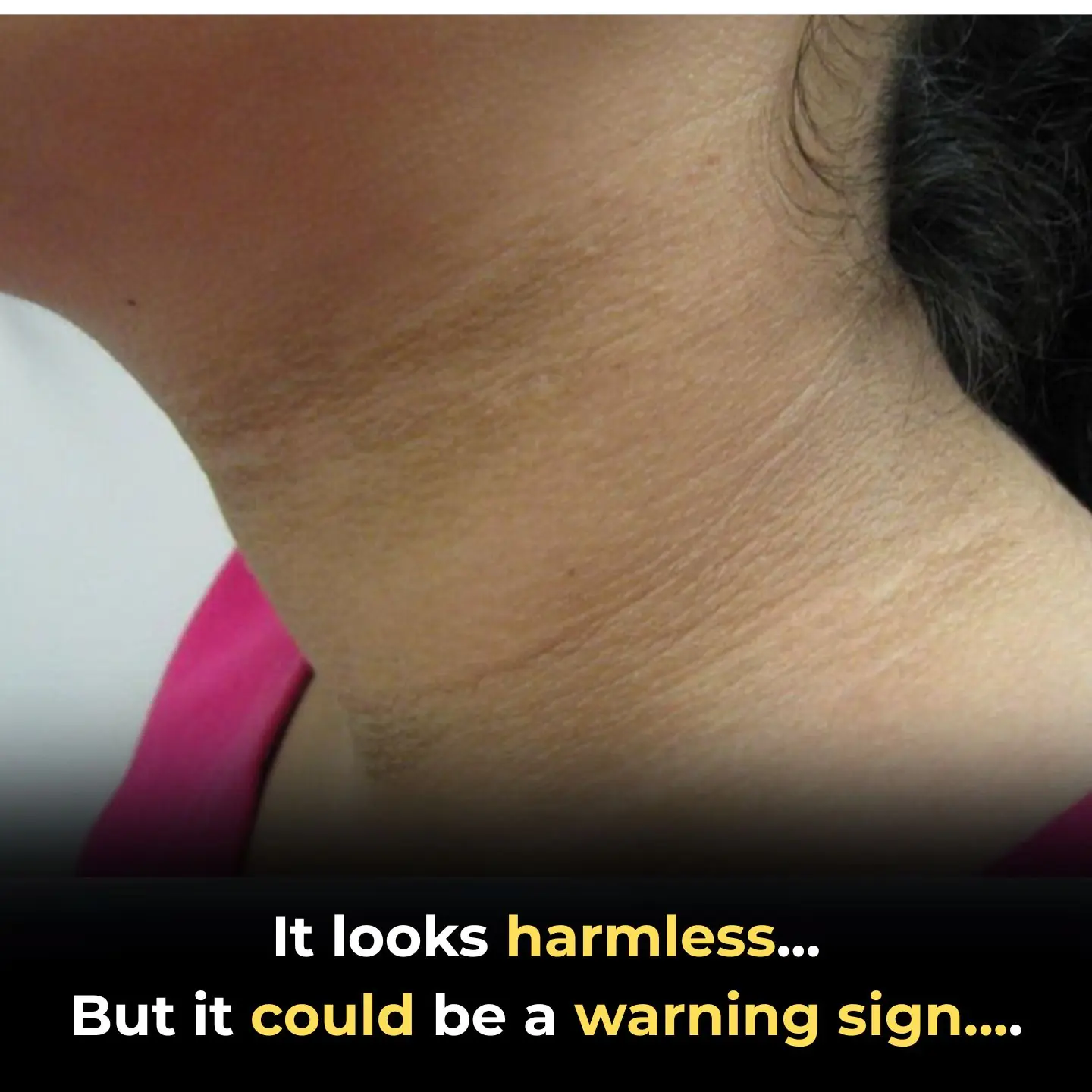
Why Your Dark Neck Isn't "Dirt": Understanding Acanthosis Nigricans

NOT JUST TIRED: A Silent Liver Signal Your Eyes Might Be Showing

Is That a Bruise or Something Else? The Silent Truth About Vertical Black Lines on Your Nails
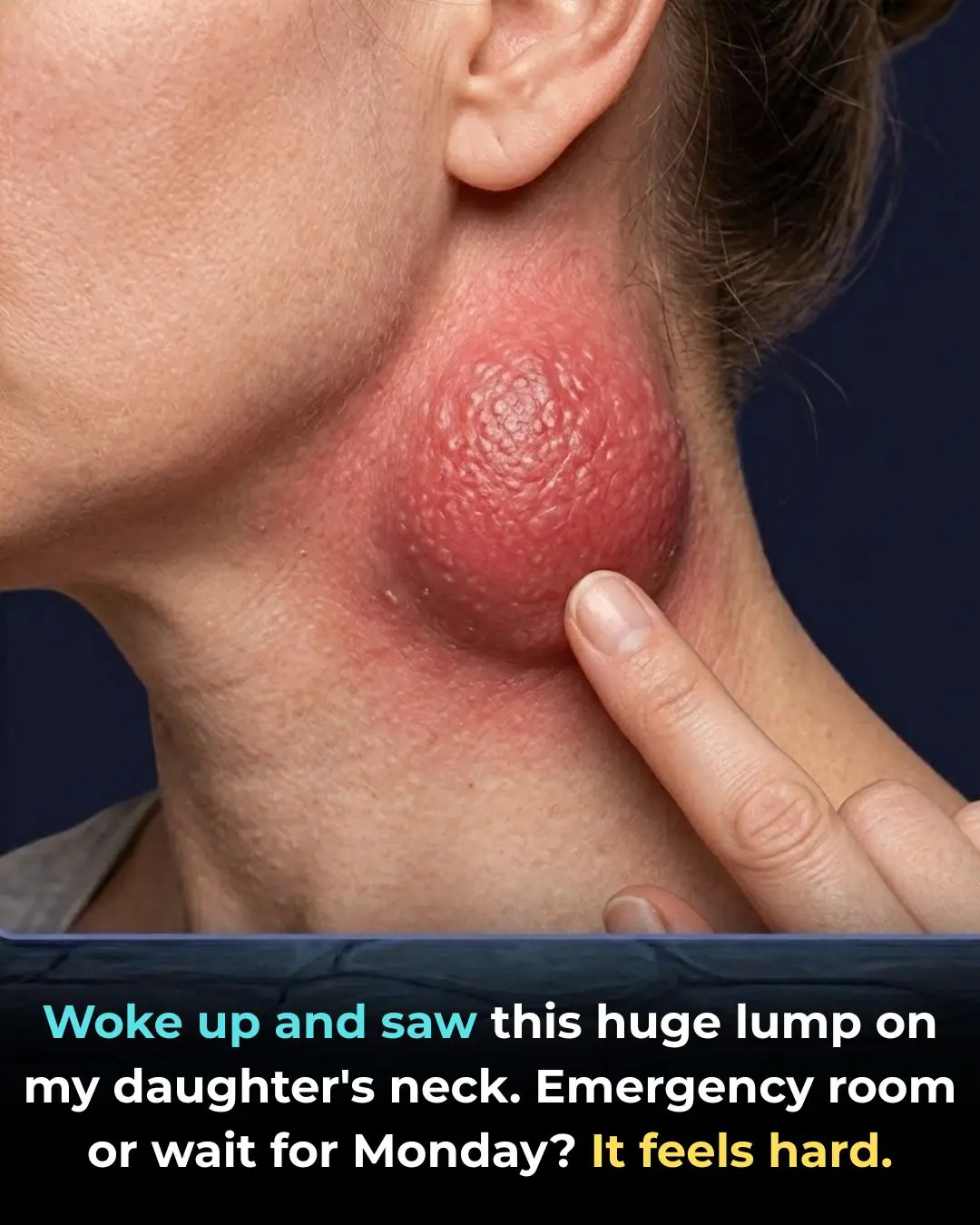
Woke up and saw this huge lump on my daughter’s neck. Emergency room or wait for Monday? It feels hard.
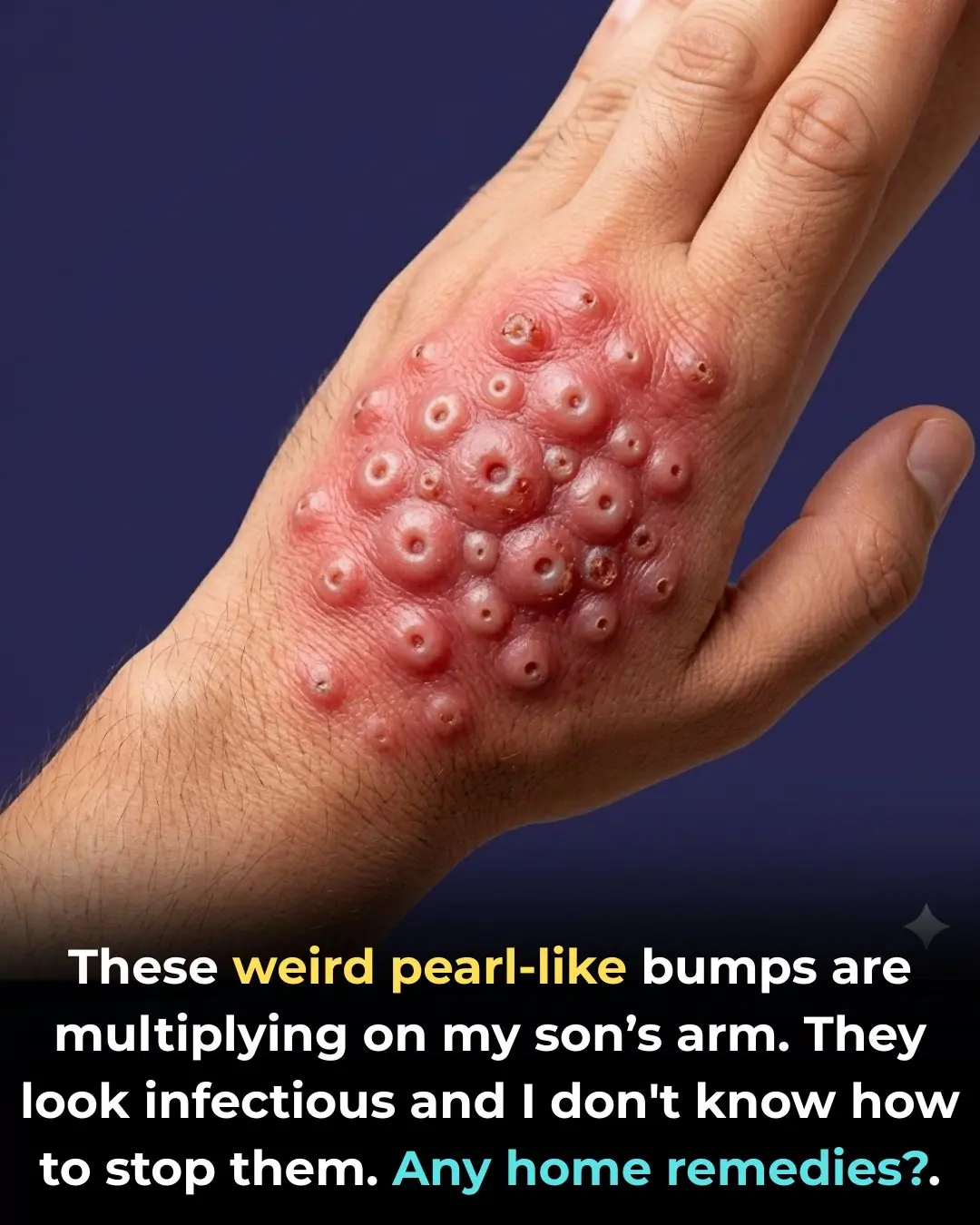
These weird pearl-like bumps are multiplying on my son’s arm. They look infectious and I don't know how to stop them. Any home remedies?

5 types of vegetables you need to pay attention to when eating them.

You probably don't know what it's called, and you may not even know about its amazing uses.
Cut Sugar from Your Diet
News Post

Most people underestimate this resin—until they discover both its extraordinary power and its astonishing price.

Biker Discovers Kidnapped Grandma Hidden in a Shipping Container, What 5,000 Motorcyclists Did Next Left the World in Tears.

A Lone Biker Was Freezing to Death Until a 76-Year-Old Grandma Grabbed His Vest and Started Dragging.

Elderly Lady Stumbles Upon 2 Injured Hell’s Angels, Her Reaction Stuns the Whole Town

Biker Hired Old Widow & Child To Cook — But She Melted The Hells Angels Boss’s Hard Heart

The Boy Who Trusted a Gangster

The first animal you see will reveal your worst flaw...

Why do some men grow this nail long?

The Millionaire’s Daughter Cried Every Day… Until the Obese Maid Discovered Something Terrible on Her Back
The First Word You See Reveals Your Most Dominant Trait

The First Three Colors You See Reveal How You INTIMIDATE People!

Waking Up Between 3 and 5 AM: What It Really Means for Your Body and Mind
Why do some men grow this nail long?

The number of circles you see will tell you if you are a narcissistic person.

Philippines Declares National Energy Emergency as President Marcos Promises Steady Oil Supply

Gold jumps 2% as oil slump eases inflation fears amid Trump Iran talks

Oil falls over 5% as Iran signals safe passage for ‘non-hostile’ ships through Strait of Hormuz

Crack the Case: Why Detective Riddles Are the Ultimate Workout for Your Brain

Why Cottage Cheese Deserves a Spot in Your Daily Diet
